GLP-1 medications — Ozempic, Wegovy, Mounjaro, Zepbound — have dramatically changed pre-surgical planning for cosmetic patients. Two distinct issues matter, and patients almost always conflate them. The first is anesthesia safety: GLP-1s slow gastric emptying, which can leave food in the stomach long after the standard "nothing by mouth after midnight" instruction and increases the risk of aspiration during induction of general anesthesia. The second is contour planning: excisional procedures (skin removal, body lifts, tummy tucks) work best on patients whose weight has plateaued, because operating mid-loss usually means a second round of skin laxity later. This guide covers both — the anesthesia hold protocols, the weight stability target, and how the answers differ depending on whether you are scheduling a body lift, a BBL, or a facelift.
Patient Education
How to Time Cosmetic Surgery Around Ozempic, Wegovy, and Other GLP-1 Medications
GLP-1 medications have changed pre-surgical planning. This guide covers both ends of the equation: anesthesia safety and weight stability.

By Dr. Gevork TatarianDouble Board-Certified Cosmetic SurgeonPublished May 8, 2026 · 10 min read · Updated May 8, 2026
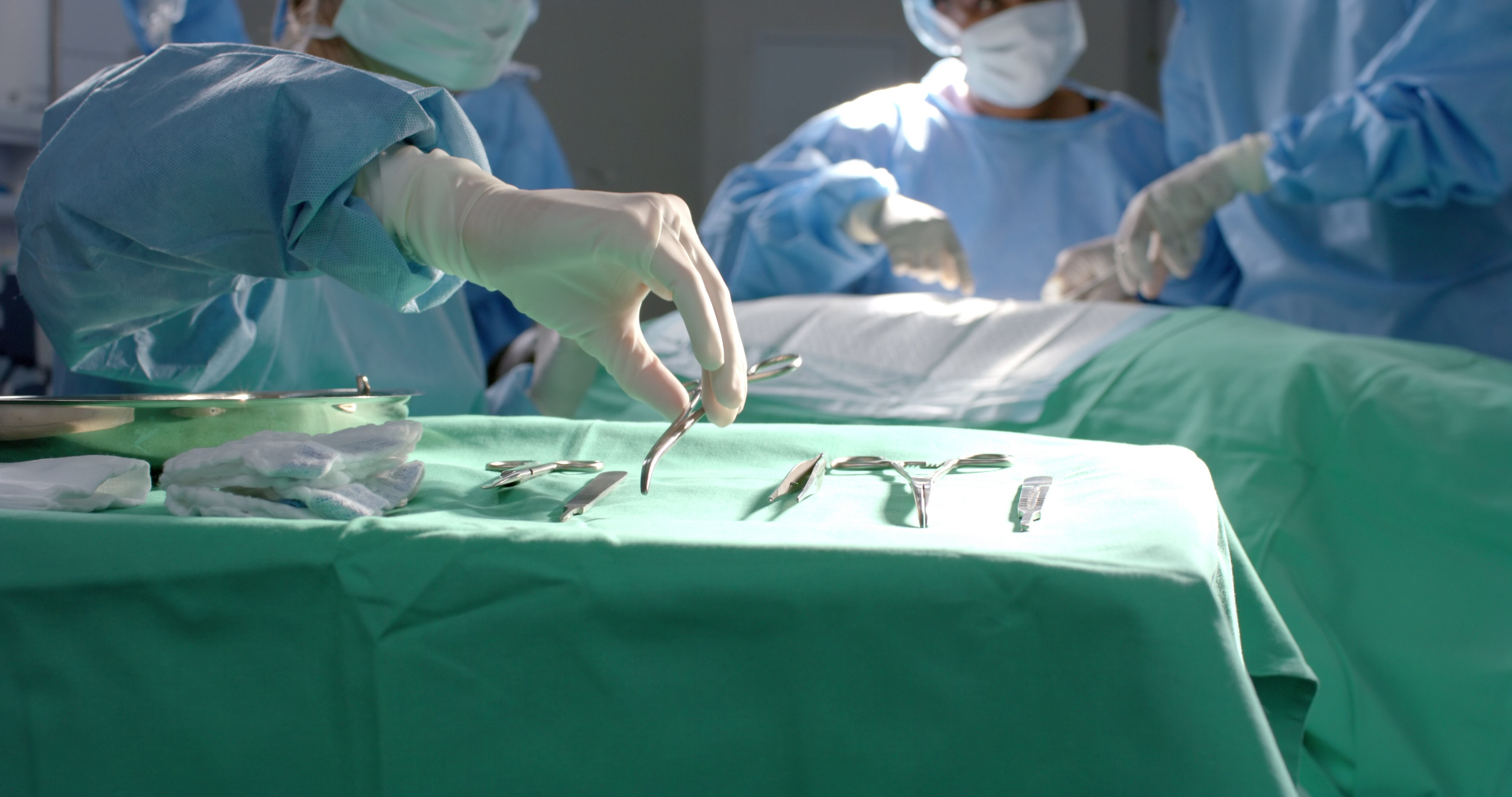
What GLP-1 Medications Do (Briefly)
- Semaglutide — sold as Ozempic (weekly, type 2 diabetes) and Wegovy (weekly, weight management).
- Tirzepatide — sold as Mounjaro (weekly, type 2 diabetes) and Zepbound (weekly, weight management). A dual GIP/GLP-1 receptor agonist.
- Mechanism: these medications mimic incretin hormones, increase insulin secretion in response to glucose, suppress appetite centrally, and — most importantly for surgery — slow gastric emptying.
- Why this matters surgically: the same slowed gastric emptying that helps with appetite control creates a real risk under general anesthesia. It also means a substantial percentage of cosmetic-surgery candidates are now arriving at consultation having lost 30-100+ pounds and needing skin-removal procedures.
The Anesthesia Risk: Delayed Gastric Emptying
- The core risk is aspiration — stomach contents entering the airway during induction of general anesthesia. Aspiration can cause chemical pneumonitis or, rarely, severe respiratory complications.
- Standard NPO instructions may not be sufficient. "Nothing by mouth after midnight" assumes a normally emptying stomach. Patients on GLP-1 medications can have measurable food residue many hours past that window.
- ASA guidance. The American Society of Anesthesiologists has issued consensus-based guidance on managing GLP-1 medications around elective surgery. Read it directly: ASA — Consensus-Based Guidance on Preoperative Management of GLP-1 Receptor Agonists.
- Guidelines are evolving. Recommendations have shifted as more data accumulates. Confirm the current hold protocol with your anesthesiologist for the date of your surgery — not the protocol that existed when you booked.
Current Pre-Op Hold Recommendations
Note: GLP-1 pre-op guidelines evolve quickly. The framework below summarizes the common practice pattern. Confirm current ASA guidance and your specific hold timing with the anesthesia team prior to surgery.
- Daily-dose GLP-1 (e.g., daily liraglutide): typically held the day of surgery.
- Weekly-dose GLP-1 (Ozempic, Wegovy, Mounjaro, Zepbound): typically held at least 1 week before surgery; some practices extend the hold longer based on dose, individual risk factors, and emerging data.
- Why protocols vary: the literature is still maturing. Some institutions favor longer holds; some emphasize point-of-care gastric ultrasound on the day of surgery; some adjust based on dose level and how recently it was escalated.
- Always disclose every medication in your pre-op intake — including injectables you may have started recently and including compounded versions of semaglutide or tirzepatide.
- Don't self-edit your medication list. Patients sometimes omit a GLP-1 from their intake because they "don't think of it as a medication." This omission can compromise your safety.
The Weight Stability Question
- Why surgeons want stable weight 3-6 months pre-op for excisional cases. The amount and pattern of skin a surgeon removes is calibrated to your current envelope. Significant weight change after the operation invalidates that calibration.
- If you keep losing post-op: the previously-tight closure becomes loose. New skin laxity emerges in the operated area. A second procedure may be needed to recapture the result.
- If you regain post-op: excess tension on the closure can widen the scar, distort contour, and stress the muscle repair (in tummy tuck patients).
- A realistic plateau before booking means at least 3 months at a stable weight (within ~5 lbs), ideally 6 months. Patients tapering off GLP-1 should generally complete the taper and demonstrate stability before booking excisional surgery.
- Patients still actively losing can usually proceed with non-excisional procedures (smaller-volume liposuction, certain breast or facial cases) but should defer body lifts and skin removal.
Surgery Types and GLP-1 Timing Sensitivity
High Sensitivity (Plan Carefully)
- Skin removal surgery — calibrated to current envelope; weight changes invalidate the plan.
- Lower body lift — circumferential closure under tension; sensitive to ongoing loss or regain.
- Arm lift (brachioplasty) — visible long incisions; loose post-op skin is unforgiving.
- Thigh lift — same issue, with closure over high-tension medial tissue.
- Panniculectomy and apron belly surgery — extent of resection is dictated by current pannus volume.
- Mommy makeover with tummy tuck — same calibration logic; muscle repair and skin removal are anchored to current anatomy.
Moderate Sensitivity
- Liposuction — removes fat cells permanently from treated areas, but ongoing weight change reshapes the surrounding zones and can produce relative contour irregularities.
- Brazilian Butt Lift — fat survival is influenced by weight stability post-op. Significant weight loss after BBL shrinks transferred fat just like native fat.
Lower Sensitivity (But Still Disclose)
- Breast surgery (augmentation, lift, reduction) and facial surgery — the contour result is less driven by total body weight, but the anesthesia hold rules apply identically. Always disclose your GLP-1 use.
- Even "small" elective procedures performed under general anesthesia or deep sedation are subject to the same aspiration risk profile.
Pre-Op Optimization on GLP-1
- Protein intake. Many GLP-1 patients are functionally protein-deficient. Aim for at least 0.8-1.0 g of protein per pound of goal body weight, and emphasize protein at every meal. Adequate protein is essential for wound healing.
- Micronutrient labs. Ask your prescribing provider or surgeon to check vitamin B12, iron studies, vitamin D, and a basic metabolic panel before booking. Deficiencies should be corrected pre-op.
- Muscle mass preservation. Significant GLP-1-driven weight loss often includes lean muscle loss. Strength is a marker of surgical resilience.
- Resistance training pre-op. 2-3 sessions per week for at least 8-12 weeks before surgery helps preserve and rebuild muscle.
- Why this matters: malnutrition — even at a "normal" body weight on the scale — increases the risk of wound dehiscence, infection, and delayed healing. A patient who looks great on paper can still heal poorly if their nutrition is depleted.
What Elevé Asks at Consultation
- Current dose and frequency of every GLP-1, including any compounded versions and any recent dose escalations.
- Duration of use — how long you have been on the medication and through how many dose increases.
- Total weight lost from peak weight, and your current BMI relative to goal.
- Trajectory — are you still losing? Plateaued? Beginning to regain after a taper?
- Plans during recovery — will you continue, hold, or taper through the recovery period?
- Coordination with the prescribing provider. If you have a separate weight-management physician, surgical timing should be coordinated across both clinicians.
After Surgery: Resuming GLP-1
- When to restart varies by procedure, your nausea level, and your prescribing provider's preference. Many patients restart between 1-4 weeks post-op.
- Early post-op nausea overlaps with GLP-1 side effects. Restarting too soon can compound nausea and reduce oral intake when adequate hydration and protein are most critical for healing.
- Hydration and protein come first. Do not restart a GLP-1 if you are still struggling to drink fluids or eat enough protein.
- Coordinate the restart with both your surgeon and the prescribing provider. A staged taper-back-up to your prior dose is often safer than resuming at full dose.
Why Choose Elevé for Post-GLP-1 Body Contouring
- Significant experience with patients after major weight loss — bariatric, GLP-1, and lifestyle. Dr. Gevork Tatarian is a double board-certified cosmetic surgeon (ABCS & ABS).
- Skin removal expertise. Body lifts, panniculectomy, brachioplasty, and thigh lifts are core operations at Elevé — not occasional add-ons.
- AAAASF-accredited surgical facility with anesthesia teams familiar with current GLP-1 hold protocols.
- Honest scheduling guidance. If you are not yet weight-stable, we will tell you to wait — even if it means deferring your booking by 6 months.
- Financing. CareCredit, Cherry, and PatientFi available; see our Insurance & Financing page for details and pre-authorization-eligible procedures.
Frequently Asked Questions
GLP-1 pre-operative guidance is evolving. Patients must disclose all medications to their surgical and anesthesia teams. Specific hold protocols are determined by the anesthesiologist based on current ASA guidance and individual patient factors. This content is educational and not medical advice.
Schedule Your Consultation
Book a consultation with Dr. Gevork Tatarian in Coral Gables. We'll review your weight trajectory, GLP-1 regimen, and goals — and tell you honestly whether now is the right time to operate, or whether a few more months of stability will produce a better long-term result.
